International Women’s Day is a moment to celebrate progress, resilience, and strength. It’s also a reminder that protecting women’s health remains essential. Many of the cancers affecting women most in the UK are influenced by lifestyle, vaccination, and screening. While no prevention strategy offers certainty, there are practical steps women can take today to lower their risk. Understanding what’s genuinely preventable empowers smarter health decisions.
Macmillan Cancer Support estimated in 2025 that in the UK, 640,000 women have been diagnosed with cancer in the previous 5 years1. This figure highlights the significant number of women currently navigating the treatment, recovery, and long-term monitoring.
While no cancer is completely avoidable, as genetics and age always play a role, there are many proactive measures you can take to lower your risk.
By focusing on prevention and prioritising early detection to catch warning signs early, you can take charge of your health. This article highlights the most effective ways for women to be proactive, stay informed, and feel empowered.
What Does “Preventable Cancer” Really Mean?
Cancer risk is a spectrum. No one is truly risk-free, but being considered high risk does not make cancer inevitable. Risk factors can be described as:
- Non-modifiable: factors that can't be changed, like age, biological sex, and genetics.
- Modifiable: behaviours that can be altered, like smoking, excessive drinking, or being overweight.
Cancer Research UK states that almost 40 per cent of cancers are preventable2. The steps you can take to reduce this risk involve reducing modifiable risk factors and taking part in vaccination and screening services where they are available.
Screening services are powerful tools to detect early signs before symptoms develop. The NHS provides nationwide screening services for breast, cervical, and bowel cancers, which are designed to identify signs as early as possible to provide the most treatment options and greatest chance of success3.
Pairing lifestyle shifts with regular screening maximises options and long-term health.
Cervical Cancer – One of the Most Preventable
Over 99 per cent of cervical cancers are caused by the Human Papillomavirus (HPV)4.
In the UK, HPV vaccines are offered to school children aged 12-13, and to women who did not receive the vaccine in school, up to age 25. The NHS also offers a cervical cancer screening service for women aged 25 to 64. This screening identifies high-risk HPV strains and detects early changes to cervical cells before they develop into a tumour5,6.
Nationwide roll-outs of the HPV vaccine and regular smear testing have increased the 5-year survival for early cervical cancer to over 95 per cent compared to 15 per cent in those who are diagnosed at a late stage7.
Lung Cancer – Largely Preventable
The main cause of lung cancer is smoking, with around 60 per cent of cases being directly linked with either first or second-hand smoke exposure8.
Although historically lung cancer affected more men, rates in women have been steadily increasing over time. While the exact cause is unknown, it is thought to be because women are more susceptible to the damage that smoking causes, putting them at higher risk9.
Quitting smoking at any age significantly reduces the risk of developing lung cancer. For non-smokers, avoiding secondhand smoke, reducing exposure to air pollution, and maintaining a healthy lifestyle can all lower your risk.
Routine screening services are not available in the UK, but knowing the early warning signs can increase the chances of being diagnosed early. Early symptoms may include10:
- Persistent cough lasting over 3 weeks
- Breathlessness
- Recurring chest infections
- Unexplained weight loss
- Fatigue
Though lung cancer is mainly caused by modifiable risk factors, genetics, age, sex, and other conditions such as chronic obstructive pulmonary disorder (COPD) also contribute to risk8. Prioritising quitting and symptom awareness empowers women to cut lung cancer risk and catch it early for better outcomes.
Bowel Cancer – Lifestyle and Screening Matter
Bowel cancer is linked to many lifestyle factors, such as11:
- Diets low in fibre and high in red or processed meats
- Obesity
- Low levels of physical activity
- Smoking
- Excessive alcohol consumption
While making healthier choices can significantly reduce risk, it does not remove it completely. Age, genetics, and previous medical history also increase the risk of developing bowel cancer11.
The NHS offers an at-home bowel cancer screening service to those aged 54 to 74. The screening programme aims to detect changes before symptoms appear, expanding treatment options12. The screening service has already reduced mortality by ~15 per cent in those who are screened vs those who do not take part13.
Taking part in screening when invited, alongside maintaining a balanced diet, staying active, limiting alcohol, and keeping a healthy weight, offers the best protection.
Breast Cancer – Partly Preventable
Breast cancer is not fully preventable, but certain lifestyle choices can influence risk.
Keeping to a healthy weight (especially after menopause), exercising, and limiting alcohol intake can all help lower the risk of developing breast cancer14.
However, non-modifiable risk factors like age, being female, family history, and genetic conditions such as the BRCA gene mutation also play a major role in increasing risk. So those who maintain a healthy lifestyle with minimal risk factors may still develop breast cancer15.
The NHS Breast Screening Programme is offered to women aged between 50 and 71, and aims to detect breast cancer before symptoms appear.
Between 1991 and 2005, the screening programme reduced deaths associated with breast cancer by 21 per cent in those screened vs those who were not. This figure has steadily risen, and in 2020 it was estimated that the screening programme reduced breast cancer-related deaths by ~37 per cent in those screened at least once16.
Regular screening, regularly checking for changes at home, and communicating with your GP about any worries that you have are all practical steps you can take to be proactive about breast cancer.
Ovarian Cancer – More Complex
Ovarian cancer has fewer modifiable risk factors compared to other cancers17.
Using the oral contraceptive pill for several years can reduce risk by up to 30–50 per cent, depending on duration of use. Having children, breastfeeding, and tubal ligation are also protective18. Maintaining a healthy weight may help with certain subtypes, though evidence on smoking is mixed – it slightly lowers risk for some ovarian cancers but increases it for others19.
Non-modifiable factors such as age (most common over 50), family history, BRCA1/2 mutations (lifetime risk up to 40–70 per cent for carriers), endometriosis, and starting periods early or late menopause play a larger role20,21.
Currently, there is no national screening programme in the UK. Therefore, the key proactive steps you should take are discussing family history or genetic testing with a GP and being aware of symptoms like:
- Persistent bloating
- Feeling full quickly
- Pelvic pain
What You Can Do Today
Understanding what is within your control is the first step you can take to reduce your cancer risks.
- Stop smoking
- Maintain a healthy weight
- Limit alcohol
- Stay active
- Eat a balanced diet
- Attend screening appointments
- Ensure HPV vaccination where eligible
The Role of Early Detection
Though modifying behaviours to lower risk is important, it is not a guarantee. Early detection and intervention save lives.
Being aware of symptoms and reporting them as early as possible is important, but symptoms often signal that the disease has already progressed.
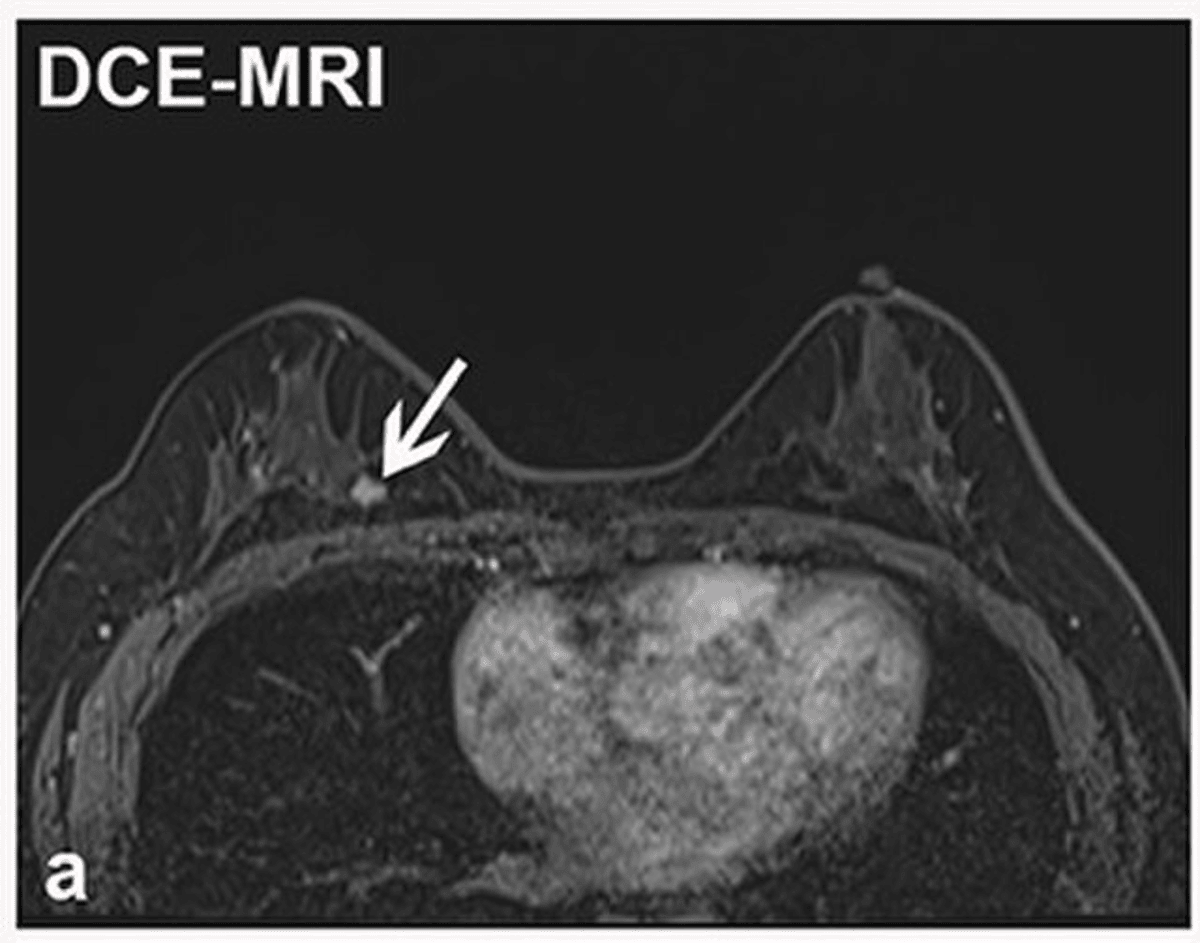
Proactive screening using imaging technologies such as MRI can give you detailed insights into several organs and detect early warning signs of cancers before they develop.
Ezra's MRI screening service can scan up to 14 organs and offers a quick, non-invasive screen by AI-assisted radiology experts. Regular screening alongside GP input can be the key to early detection and peace of mind when it comes to your health.
Conclusion
While no cancer is entirely preventable, many affecting women have strong modifiable components through vaccination, lifestyle changes, and screening services. Small, consistent actions today can empower women to lower risks, catch issues early, and maximise treatment success.
This International Women's Day, consider proactive options like Ezra's MRI scans alongside GP guidance for peace of mind. Book your scan today.
Understand your risk for cancer with our 5 minute quiz.
Our scan is designed to detect potential cancer early.
References
1. Macmillan Cancer Support. Cancer prevalence - Macmillan Cancer Support. Accessed March 2, 2026. https://www.macmillan.org.uk/about-us/what-we-do/research/cancer-prevalence
2. Cancer Research UK. Cancer Stats Data Hub. September 26, 2025. Accessed January 12, 2026. https://crukcancerintelligence.shinyapps.io/CancerStatsDataHub/_w_defe7cc6a05e447ca04d766f7c099545/_w_0bf5a94f00034809a2181d2fb80fd08b/?_inputs_&nav=%22Incidence%20Breakdowns%20and%20Trends%22&app_select_CancerSite=%22Cervix%22&app_select_Country=%22United%20Kingdom%22
3. Macmillan Cancer Support. Cancer screening - Macmillan Cancer Support. Accessed March 3, 2026. https://www.macmillan.org.uk/cancer-information-and-support/worried-about-cancer/screening
4. Cancer Research UK. The HPV vaccine | Cancer Research UK. Accessed January 16, 2026. https://cancerresearchuk.org/about-cancer/causes-of-cancer/infections-eg-hpv-and-cancer/the-hpv-vaccine
5. Cancer Research UK. Risks and causes of cervical cancer. Accessed January 16, 2026. https://www.cancerresearchuk.org/about-cancer/cervical-cancer/risks-causes
6. NHS. Human papillomavirus (HPV). nhs.uk. March 19, 2019. Accessed January 16, 2026. https://www.nhs.uk/conditions/human-papilloma-virus-hpv/
7. Cancer Research UK. Survival for cervical cancer. September 21, 2023. Accessed January 12, 2026. https://www.cancerresearchuk.org/about-cancer/cervical-cancer/survival
8. Cancer Research UK. Risks and causes of lung cancer. Accessed March 3, 2026. https://www.cancerresearchuk.org/about-cancer/lung-cancer/risks-causes
9. Gee K, Yendamuri S. Lung cancer in females—sex-based differences from males in epidemiology, biology, and outcomes: a narrative review. Transl Lung Cancer Res. 2024;13(1):163-178. doi:10.21037/tlcr-23-744
10.NHS. Lung cancer - Symptoms. nhs.uk. October 23, 2017. Accessed March 3, 2026. https://www.nhs.uk/conditions/lung-cancer/symptoms/
11.Cancer Research UK. Risks and causes of bowel cancer. Accessed March 3, 2026. https://www.cancerresearchuk.org/about-cancer/bowel-cancer/risks-causes
12.NHS. Bowel cancer screening. nhs.uk. October 20, 2017. Accessed February 2, 2026. https://www.nhs.uk/tests-and-treatments/bowel-cancer-screening/
13.Logan RFA, Patnick J, Nickerson C, Coleman L, Rutter MD, von Wagner C. Outcomes of the Bowel Cancer Screening Programme (BCSP) in England after the first 1 million tests. Gut. 2012;61(10):1439-1446. doi:10.1136/gutjnl-2011-300843
14.Cancer Research UK. Reducing your risk of breast cancer. Accessed March 3, 2026. https://www.cancerresearchuk.org/about-cancer/breast-cancer/risks-causes/reducing-breast-cancer-risk
15.Cancer Research UK. Breast cancer risk | Cancer Research UK. Accessed January 23, 2026. https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/breast-cancer/risk-factors
16.Johns LE, Coleman DA, Swerdlow AJ, Moss SM. Effect of population breast screening on breast cancer mortality up to 2005 in England and Wales: an individual-level cohort study. Br J Cancer. 2017;116(2):246-252. doi:10.1038/bjc.2016.415
17.Ali AT, Al-ani O, Al-ani F. Epidemiology and risk factors for ovarian cancer. Menopause Rev Menopauzalny. 2023;22(2):93-104. doi:10.5114/pm.2023.128661
18.Ferris JS, Daly MB, Buys SS, Genkinger JM, Liao Y, Terry MB. Oral contraceptive and reproductive risk factors for ovarian cancer within sisters in the breast cancer family registry. Br J Cancer. 2014;110(4):1074-1080. doi:10.1038/bjc.2013.803
19.Minlikeeva AN, Cannioto R, Jensen A, et al. Joint exposure to smoking, excessive weight, and physical inactivity and survival of ovarian cancer patients, evidence from the Ovarian Cancer Association Consortium. Cancer Causes Control CCC. 2019;30(5):537-547. doi:10.1007/s10552-019-01157-3
20.Cancer Research UK. Risks and causes of ovarian cancer. Accessed March 3, 2026. https://www.cancerresearchuk.org/about-cancer/ovarian-cancer/risks-causes
21.Mokhber A, Stewart B, Terry KL, et al. Endometriosis in Carriers of a Pathogenic Variant in BRCA1 or BRCA2: A Descriptive Analysis of a Large Multicentral BRCA Carrier Cohort. Curr Oncol. 2025;32(12):675. doi:10.3390/curroncol32120675